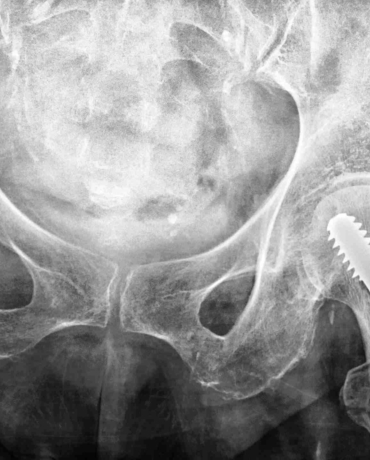
Fracture recovery
Falls are the leading cause of injury-related hospitalisation in people aged 65 and over. Our research is focused on improving fall-related hip fracture treatment.
Falls are the leading cause of injury-related hospitalisation in people aged 65 and over. Our research is focused on improving fall-related hip fracture treatment.

Factors that make a hip fracture more likely include:
The Australian and New Zealand Hip Fracture Registry (ANZHFR) is a clinician-led audit of hip fracture care established to provide data that will inform practice and drive better hospital care for people with a hip fracture. Established in 2015, the Registry stores data collected by participating hospitals and provides a mechanism for service providers to use this data to drive change in practice at a local level and ultimately to improve the care and optimise outcomes for older people who have fractured their hip.
Our research has shown that across New South Wales, there is significant variation in the time older people have to wait for their hip fracture surgery, with the conclusion that more could be done to expedite care.
Our other research in the same area has demonstrated that a particular approach to caring for hip fracture patients is associated with a lower 30-day mortality rate. When orthopaedic surgeons and geriatricians look after a hip fracture patient together, the outcomes seem to be better for older people. This approach to care is being recommended across Australia.

Principal Research Fellow, NeuRA (Conjoint)
Every dollar of community support enables our scientists to continue making life-changing discoveries that contribute to a brighter and healthier future.
Run, swim or bake your way to making a positive difference in the lives of people touched by brain and nervous system disorders.
Stay informed about our latest research breakthroughs, scientific discoveries and the incredible minds behind them – subscribe today.
Neuroscience Research Australia respectfully acknowledges the Bidjigal and Gadigal peoples of the Eora Nation as the Traditional Owners of the Land on which we stand and pay our respects to Elders past and present.
Redevelopment of the NeuRA website has been made possible by the generous support of Conexus Financial.